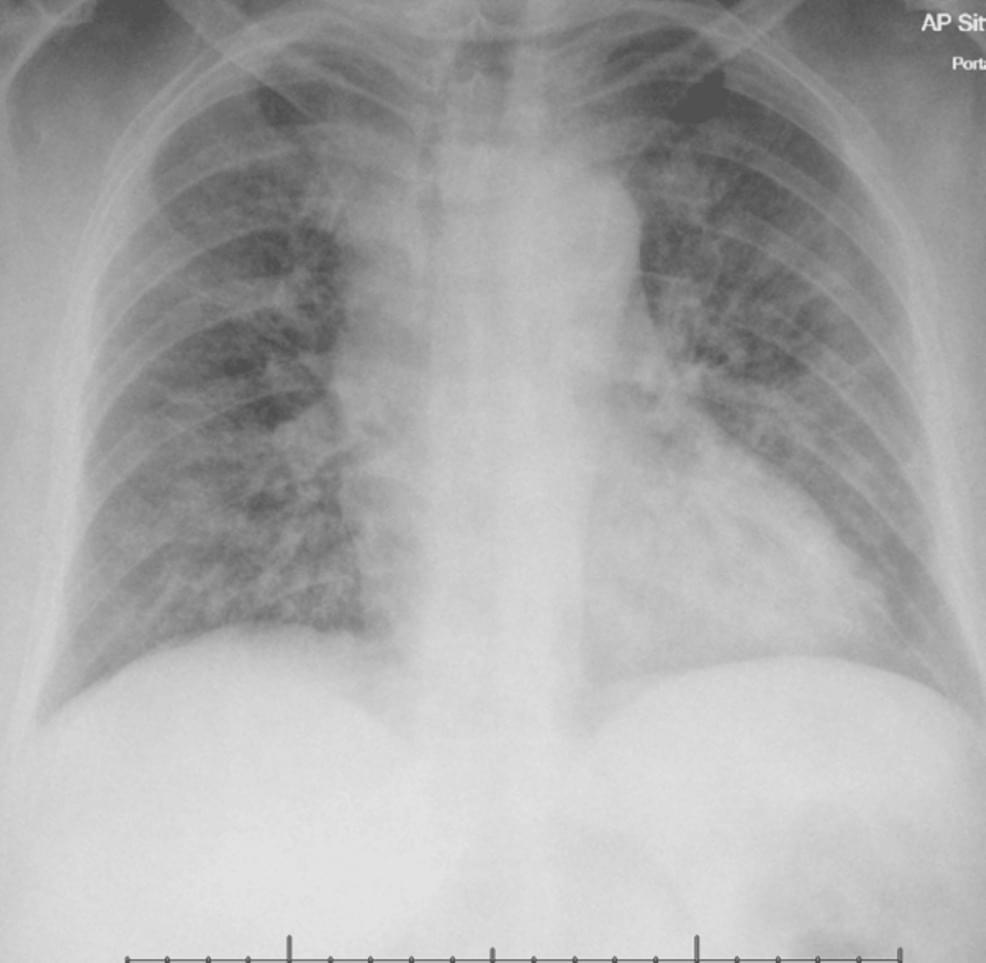
This stage IV lung cancer patient developed: persistent fever thrombocytopenia multiorgan dysfunction steroid-refractory course.
A high H-score led to the diagnosis: ICI-associated HLH. She improved rapidly with anakinra after failing steroids.
Takeaway: In immunotherapy patients, extreme hyperferritinaemia should trigger HLH evaluation early.
Would you have escalated to anakinra…or tried second-line steroids first?
Read more here.
Immune checkpoint inhibitors (ICIs) are increasingly used in advanced malignancies but can cause rare, severe immune-related adverse events (irAEs). Haemophagocytic lymphohistiocytosis (HLH) is a life-threatening hyperinflammatory syndrome infrequently reported with ICIs and often challenging to diagnose. We report a case of a woman in her 60s with stage IV lung adenocarcinoma treated with pembrolizumab-based chemoimmunotherapy who developed recurrent, steroid-refractory immune-related hepatitis and pneumonitis. Twenty-four weeks after starting pembrolizumab, she presented with persistent fever, thrombocytopenia, extreme hyperferritinaemia (ferritin >33,500 µg/L), and progressive multiorgan dysfunction. Despite overlap with other irAEs and infection, a high H-score prompted evaluation for HLH, confirmed on bone marrow biopsy with haemophagocytosis.