Whole genome sequencing is powerful but still very new. Many companies offer genetic predictions for diseases without clearly explaining how those models are built or validated. Most people don’t ask basic questions like: How accurate is this? What data was used? What are the limitations? In this video, we break down why transparency matters and why you should always question genetic risk scores before trusting them. Youtube Video: https://www.youtube.com/LongevityScienceNews/membership Patreon: https://www.patreon.com/posts/polygenic-scores-152170836?utm…=join_link https://www.herasight.com/
Category: biotech/medical – Page 73
Three anesthesia drugs all have the same effect in the brain, MIT researchers find
When patients undergo general anesthesia, doctors can choose among several drugs. Although each of these drugs acts on neurons in different ways, they all lead to the same result: a disruption of the brain’s balance between stability and excitability, according to a new MIT study.
This disruption causes neural activity to become increasingly unstable, until the brain loses consciousness, the researchers found. The discovery of this common mechanism could make it easier to develop new technologies for monitoring patients while they are undergoing anesthesia.
“What’s exciting about that is the possibility of a universal anesthesia-delivery system that can measure this one signal and tell how unconscious you are, regardless of which drugs they’re using in the operating room,” says Earl Miller, the Picower Professor of Neuroscience and a member of MIT’s Picower Institute for Learning and Memory.
Miller, Edward Hood Taplin Professor of Medical Engineering and Computational Neuroscience Emery Brown, and their colleagues are now working on an automated control system for delivery of anesthesia drugs, which would measure the brain’s stability using EEG and then automatically adjust the drug dose. This could help doctors ensure that patients stay unconscious throughout surgery without becoming too deeply unconscious, which can have negative side effects following the procedure.
Miller and Ila Fiete, a professor of brain and cognitive sciences, the director of the K. Lisa Yang Integrative Computational Neuroscience Center (ICoN), and a member of MIT’s McGovern Institute for Brain Research, are the senior authors of the new study, which appears today in Cell Reports. MIT graduate student Adam Eisen is the paper’s lead author.
Excellent work Earl Miller and team!
Read More
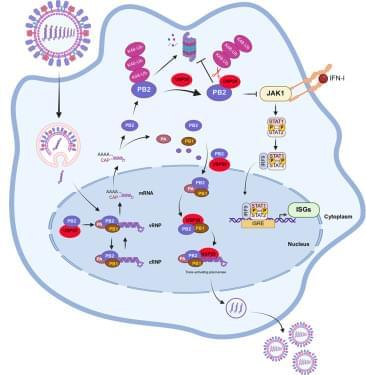
Dual roles of USP39 in stabilizing PB2 and orchestrating ribonucleoprotein assembly drive H5 influenza virus replication and pathogenicity
Yang et al. identify USP39 as a deubiquitinase hijacked by H5 AIV. USP39 catalytically deubiquitinates PB2 to prevent its degradation and maintain polymerase activity. Meanwhile, it promotes PB2-PB1 association for RNP assembly. The dual-function mechanism facilitates viral replication, enhances pathogenicity, and represents a promising anti-H5 therapeutic target.
Early adult drinking linked to middle-age cognitive decline—even after extended abstinence
It’s well known that alcohol consumption is an age-old method for coping with stress. But recent research led by the University of Massachusetts Amherst has found that when such self-medication begins in early adulthood, negative cognitive effects start to show up in middle age—even after long periods of total abstinence. The study is published in the journal Alcohol, Clinical and Experimental Research.
These negative effects include a decreased ability to cope with changing situations, an increased likelihood to drink when stressed, and the kinds of cognitive decline associated with dementia and Alzheimer’s disease. The new research helps us understand how alcohol rewires the brain’s circuitry and can help suggest new approaches for helping people adapt to the long-term effects of alcohol use.
Researchers have long known that stress and alcohol have a mutually reinforcing relationship: Alcohol can help take the edge off stressful situations, but in so doing it can decrease the brain’s ability to manage stress on its own, meaning one has to keep drinking, and drinking more, in order to relieve stress from a bad day. At the same time, the more one drinks, the more stress can accrue from increasingly poor decision-making. It can be a vicious cycle that gets harder to break the more the brain’s circuitry changes. But what about the long-term effects of stress and alcohol?
New hope for treating a rare genetic disease before birth
Stanford Medicine scientists are launching a clinical trial of prenatal transplants, using stem cells from the mother, to treat a rare genetic disease called Fanconi anemia before a baby is born.

New Data Centers Will Be Powered by Human Brain Cells
Now, Cortical Labs is ready to scale up the operation. As Bloomberg reports, the company says it’s working on “biological data centers” in Melbourne, Australia, and Singapore. Simply put, instead of relying on Nvidia chips like AI companies, Cortical Labs is planning to outfit its futuristic facilities with racks of CL1 biological computers, powered by many more human brain cells, instead.
The company refers to this approach as “wetware,” an unsettling new take on software and hardware terminology. Simply put, the computers send electrical signals to neurons derived from human blood stem cells. The chips embedded within record those neurons’ responses as the output.
The company teamed up with DayOne Data Centers, to develop the two facilities. The Melbourne data center will house 120 CL1 units, while DayOne is planning to deploy as many as 1,000 units at the one in Singapore.
Was William James Right About Consciousness?
Dr. Nicolas Rouleau is a neuroscientist, bioengineer, and Assistant Professor of Health Sciences at Wilfrid Laurier University. He wrote the award-winning essay, ‘An Immortal Stream of Consciousness: The scientific evidence for the survival of consciousness after permanent bodily death,’ in which he argues that the transmissive theory of consciousness may actually be more consistent with emerging scientific insights than the dominant assumption that the brain generates consciousness.
In this conversation with Hans Busstra, Rouleau shares the main arguments from his essay, which touch upon his collaboration with Dr. Michael Persinger, the inventor of the ‘God Helmet,’ and his work with Michael Levin on ‘mind blindness’—the idea that science may be searching for mind in too restricted a place by focusing almost exclusively on neurons.
More information on Dr. Nic Rouleau:
https://www.wlu.ca/academics/facultie… website: https://www.rouleaulab.com/ Further reading and scientific references discussed in this video: Rouleau’s BICS Essay: ‘An Immortal Stream of Consciousness: The scientific evidence for the survival of consciousness after permanent bodily death.’ https://www.bigelowinstitute.org/inde… Rouleau, N., Levin, M., et al. (2025) (Preprint; forthcoming in Philosophical Transactions of the Royal Society). Brains and Where Else? Mapping Theories of Consciousness to Unconventional Embodiments. https://tinyurl.com/439rrn8z Rouleau, N., & Levin, M. (2023). The Multiple Realizability of Sentience in Living Systems and Beyond. eNeuro, 10(11). https://tinyurl.com/2s4bdtmm Rouleau, N. & Cimino, N. (2022). A Transmissive Theory of Brain Function: Implications for Health, Disease, and Consciousness. NeuroSci, 3. https://www.mdpi.com/2673-4087/3/3/32 McCraty, R., et al. (2018). Long-term study of heart rate variability responses to changes in the solar and geomagnetic environment. https://tinyurl.com/254x3b9t Rouleau, N., & Persinger, M. A. (2016). Differential responsiveness of the right parahippocampal region to electrical stimulation in fixed human brains: Implications for historical surgical stimulation studies. Epilepsy & Behavior, 60181–186. https://tinyurl.com/uc5jbr Rajaram, M., & Mitra, S. (1981). Correlation between convulsive seizure and geomagnetic activity. Neuroscience Letters, 24, 187–191. https://tinyurl.com/3snrs4cs Chapters 0:00 Introduction 4:00 What Nic Rouleau would say to William James about his theory of transmissive consciousness 7:14 What do we know empirically about how electromagnetic fields influence our brains? 10:27 How scientifically rigorous are the empirical data on the influence of the Earth’s magnetic field on brains? 11:35 On Nic’s mentor, Dr. Michael Persinger, the inventor of the God Helmet 14:42 Research on post-mortem brain tissue 18:09 What mental states are influenced by magnetic fields? 18:58 Electromagnetic effects in dead vs. living brains 19:45 On Michael Levin and the paradigm shift due to bioelectricity 21:24 Influencing the thoughts of deceased people 25:33 Are biological forms stored in the Earth’s magnetic field? 30:21 Shielding brains from electromagnetic fields 33:12 Mind blindness: we only see 1% of the minds out there 38:55 What is the best way out of mind blindness? 41:06 Plant-based computation 42:00 The Self-Organizing Units Lab (SOUL) and what Nic is working on 43:23 Minds in a Petri dish 46:13 What counts as embodiment? 48:44 Phenomenal consciousness on different levels 53:06 What theories of consciousness can get us out of the behaviorist trap? 57:25 Nic’s award-winning essay on consciousness beyond death 1:00:55 Intermediary states of consciousness, the Bardo Thodol 1:04:46 Consciousness when the radio, the brain, is completely broken 1:06:35 Why exactly is electromagnetism a better explanation of consciousness beyond death than NDEs or OBEs? 1:11:58 How does the God Helmet work? 1:17:31 Which electromagnetic fields influence our consciousness and which ones don’t? 1:23:59 Can all of consciousness be stored in the Earth’s magnetic field? 1:27:08 Children with past-life memories: could electromagnetism play a role there? 1:29:51 How do quantum theories of consciousness relate to the work of Nic? 1:33:42 Do our brains connect electromagnetically with each other? 1:35:28 Nic on the hard problem of consciousness 1:38:00 Aren’t you just a materialist 2.0? 1:40:25 On the meaning of Nic’s work Copyright © 2026 Essentia Foundation. All rights on interview content reserved.
Personal website: https://www.rouleaulab.com/
Further reading and scientific references discussed in this video:
Rouleau’s BICS Essay: ‘An Immortal Stream of Consciousness: The scientific evidence for the survival of consciousness after permanent bodily death.’ https://www.bigelowinstitute.org/inde…
Rouleau, N., Levin, M., et al. (2025) (Preprint; forthcoming in Philosophical Transactions of the Royal Society). Brains and Where Else? Mapping Theories of Consciousness to Unconventional Embodiments. https://tinyurl.com/439rrn8z.
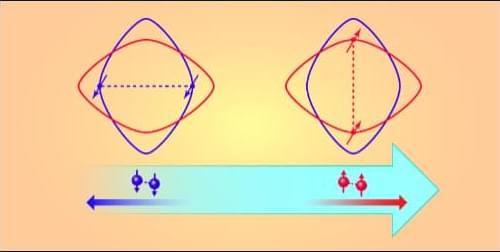
Spin Supercurrents in Superconducting Altermagnets
Materials from a new class of magnets could host permanent dissipationless spin currents when they enter a superconducting state.
Superconductors are famous for transporting electric charge with zero resistance. This ability underpins technologies such as MRI scanners, quantum computers, and sensitive magnetometers known as superconducting quantum interference devices. However, in the field of spintronics—which seeks to process information using electron spin rather than charge—achieving a similar long-range dissipationless transport has remained elusive. In ordinary metals, electron spins are highly susceptible to scattering and spin-orbit coupling, both of which cause spin currents to decay over short distances. Although research in superconducting spintronics based on ferromagnets has made progress [1, 2], ferromagnets produce stray magnetic fields that interfere with external circuit elements, and their internal magnetic fields tend to destroy superconductivity.

Ryugu asteroid samples contain all DNA and RNA building blocks, bolstering origin-of-life theories
All the essential ingredients to make the DNA and RNA underpinning life on Earth have been discovered in samples collected from the asteroid Ryugu, scientists said Monday.
The discovery comes after these building blocks of life were detected on another asteroid called Bennu, suggesting they are abundant throughout the solar system.
One longstanding theory is that life first began on Earth when asteroids carrying fundamental elements crashed into our planet long ago.
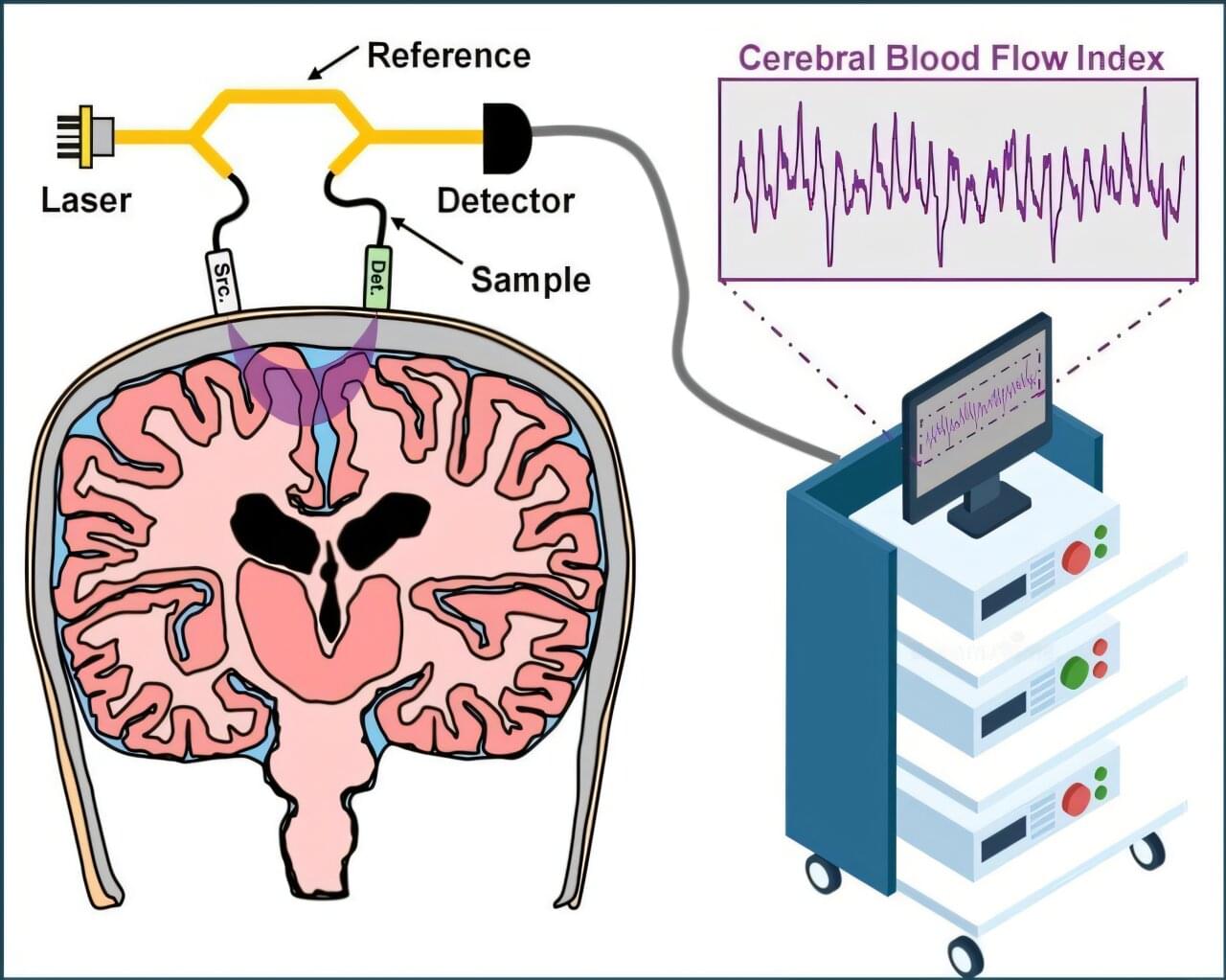
Next-gen interferometric diffusing wave spectroscopy achieves 20x signal boost in cerebral blood flow monitoring
Cerebral blood flow is essential for normal brain function and often perturbed in neurological disease. If one shines a source of coherent light on perfused tissue, the detected speckles, or “grains” of light fluctuate, or “dance,” at a rate proportional to blood flow in the volume sampled by the light. In brain tissue, this concept can be harnessed to measure the cerebral blood flow index (CBFi).
However, to date, implementations of this principle for noninvasive adult human brain monitoring—collectively known as diffuse correlation spectroscopy (DCS)—have achieved limited brain sensitivity. This is because the brain is 1–2 centimeters deep beneath the scalp and skull, meaning that the light must sample the superficial tissue before reaching the brain.
While the collection points can be moved further from the source to address this issue by improving sampling of the brain, this strategy requires many photon-counting channels to detect highly attenuated light far from the source. DCS becomes prohibitively expensive as the number of channels increases.